Behavioral activation is a treatment for depression that has been found to be very effective, even for clients who have not had success with other approaches. Researchers have found behavioral activation to be on par with medication and slightly superior to cognitive therapy in the treatment of depression. Behavioral activation shifts away from cognitions and feelings to focus on a client's behavior and environment. This treatment guide presents an overview of the technique's theoretical underpinnings, it describes how to use behavioral activation with clients, and it provides the tools you'll need, including worksheets and video.
Theory
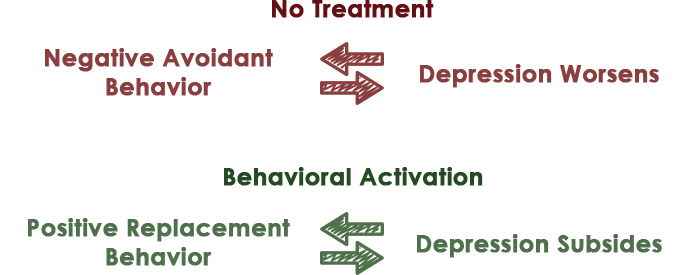
The behavioral activation model suggests that negative life events such as grief, trauma, daily stressors, or a genetic predisposition to depression can lead to a person having too little positive reinforcement. Additionally, a person might turn to unhealthy behaviors--drug use, sleeping late into the afternoon, social withdrawal, etc.--in an attempt to avoid the negative feelings. These behaviors provide temporary relief, but ultimately result in more negative outcomes, and worsening depression.
When using behavioral activation, a clinician intervenes in two primary ways: They increase the amount of positive reinforcement a person experiences, and they end negative behavior patterns that cause depression to worsen. Replacing negative avoidant behaviors with new rewarding behaviors increases a person's positive reinforcement and reduces negative reinforcement.
Using Behavioral Activation
Educating Clients
The goal of behavioral activation might seem simple (just replace negative behaviors with positive alternatives), but its implementation in real life comes with challenges. Imagine being in immense pain and having a tool that allows you to immediately relieve that pain. Now, imagine you have a tool that you hear will help more in the long run, but it isn't going to relieve the pain you're experiencing right now. Behavioral activation is the tool that will help in the long-run, but there won't be any instant relief. Unhealthy avoidant behaviors are the tools that provides instant relief, but ultimately do more harm than good. Because the goals of behavioral activation can be unclear to a client, education is an important first step.
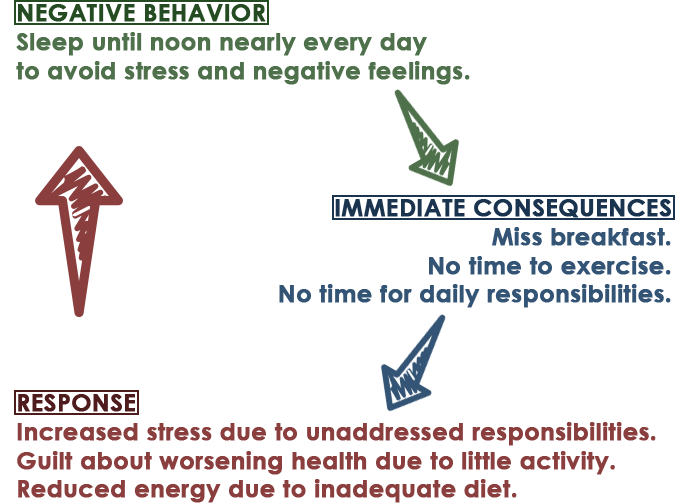
Clients who do not understand the reasoning behind behavioral activation are unlikely to be motivated to follow through. How is going out with friends or going for a walk going to help in the long-run when they still feel miserable doing these things? Why shouldn't they stay home in bed when that's the one thing that makes them feel better? It's the clinician's job to help a client recognize how their avoidant behavior (in this example, staying at home in bed) is causing their depression to worsen. This requires a clinician to listen, pinpoint negative behavior patterns, and collaborate with a client to figure out how they can be damaging. It can be helpful to draw a quick diagram, as shown below.
Developing Positive Replacement Behaviors
After educating a client about behavioral activation and identifying some negative behavior patterns, the next step is to come up with some positive replacement behaviors. This can't be emphasized enough: The positive replacements should be both easy and rewarding. Someone who is depressed might have a hard time getting out of bed by noon and brushing their teeth, let alone waking up at 6 AM, creating a résumé, or running a 10K. It can be helpful to create a list of positive rewarding behaviors, and rank them from 1 to 10 in the areas of ease and reward. Below are two worksheets to help with the process.
Implementing the Behavioral Activation Plan
Next, the clinician should work with their client to plan how and when when to complete their positive replacement behaviors. This means talking about possible obstacles, scheduling times for activities throughout the week, and deciding how the client will remember to follow through with their plan. Be specific. Don't let a client say "I'll do something on Thursday" and leave it at that. What will they do on Thursday? When exactly? How will they remember? Here's how the conversation might look.
Therapist: "What might stop you from going for a walk this week?"
Client: "Well, it might be rainy or cold... I guess I could go to the gym if that's the case."
Therapist: "Good idea! If you schedule your walking, you'll be more likely to follow through. What time can you do this?"
Client: "Right after dinner will be best--about 6:30."
Therapist: "Last question: How are you going to remember to do this? Could you leave yourself a note or set an alarm?"
Client: "Sure, I'll set an alarm on my phone right now."
Therapist: "Perfect! Remember, when the time comes, you might want to skip your walk and stay home. It's important that you push through that feeling and go."
One of the best tools for helping a client follow through with their behavioral activation plan is social support. Ask the client to choose a friend who they are comfortable talking to about their plan, and see if the friend will help encourage them. It can be helpful for the clinician to check in on a client and their plan, especially if there's a long gap between sessions.
The clinician's job doesn't end once the client begins to initiate their plan. At the beginning of every session the clinician should ask about how the client's plan is going to highlight its importance. The client's successes should be met with praise, and failures should be addressed with problem-solving. Maybe the planned activity wasn't a good fit (Was it rewarding? Was it easy?), or maybe the client just forgot to do it. If a client was successful, they should be reminded that this is a long-term project and they need to continue the following week. When motivation and mood start to improve, begin transitioning to more challenging positive activities with long-term payoffs (but don't totally neglect the easy and rewarding stuff).
That's it—you're finally done! If necessary, a client may be more able to move on and address things like negative cognitions at this point in treatment, but that's another beast altogether. Below we've included a video to further drive home some of the more important points of behavioral activation. Good luck out there, fighting the good fight against mental illness!
